
What Is Blepharitis?
Blepharitis is inflammation of the eyelids. It’s a common cause of sore, red and crusty eyelids. Blepharitis leads to an irregular tear. What we have found here at Adelaide City Optometrist is that 30-50% of our patients have reported blepharitis symptoms at some time. The tear film protects and lubricates the eyes; poor tear film quantity and quality can lead to the following signs and symptoms.
Blepharitis Signs & Symptoms
- Discomfort due the eyelids chafing on dry patches on the surface of the eye. Usually a gritty or prickly sensation, sometimes feeling itchy, tired or heavy.
- Reduced vision due to the tear film being uneven or cloudy. This causes vision to appear smeary or blurry.
- Reflex tearing, running watering eyes due to the irritation of the dry patches on the surface of the eye.
- Difficulty opening the eyes in the morning.
- Sensitivity to wind and air conditioning, generally at the start of the day going for a morning walk or starting the day in front of the computer.
- Superficial eye infections, such as blepharitis and conjunctivitis are most common.
- Crusty eyelids, where mucous is secreted by the meibomian tear glands along the eyelid margin near the base of the eye lashes. The build-up of the secretion leads to flaky, crusty eyelids.
Depending on your scenario, you might have some or all of these symptoms. Blepharitis might also be intermittent or a chronic condition. With severe cases of blepharitis, this may lead to your lashes falling out (Madarosis). We use the OSDI to further distinguish your severity of dry eye from a normal eye.
Causes
Blepharitis and dry eyes often occur at the same time. This causes confusion as to whether dry eyes causes blepharitis, or blepharitis causes dry eyes. There are several causes of blepharitis including:
- Bacterial eyelid infection
- Meibomian Gland Dysfunction (MGD)
- Fungal eyelid infection
- Parasites (Demodex) eye lash mites
Blepharitis is associated with overgrowth of bacteria that live along the margins of our eyelids and the eyelashes. Over time these bacteria multiply and create a biofilm at the base of eyelashes. This biofilm becomes a toxic environment just like the plaque that forms around your teeth. Parasitic eyelash mites feed on this biofilm. This leads to overgrowth of the eyelid mites and a worsening of the eyelid inflammation. Secondly, the bacteria in the biofilm produce exotoxins which cause inflammation in oil-secreting tear glands known as the meibomian glands. This causes a condition known as Meibomian Gland Dysfunction (MGD), leading to worsening of eye symptoms and dry eyes.
Blepharitis is often associated with other systemic skin conditions. Often our patients that appear with skin conditions such as rosacea, eczema, psoriasis, dandruff and ocular rosacea, also exhibit blepharitis.
Dry Eye Diagnostic Tests at Adelaide City Optometrist
Tear Osmolarity
IPEN diagnostic device is a quick way to measure tear osmolarity. The constant among all dry eye sufferers is tear hyper-osmolarity.
The challenge for optometrists in measuring dry eye is to find an objective measure of its severity. The IPEN allows for a quick diagnosis and more importantly allows for an objective and reliable measure of the severity of dry eye. It is also very useful in letting the optometrist know if the treatment protocol is working.
Tear Break Up Time (TBUT)
This is a clinical eye test used to assess evaporative dry eye disease. To measure TBUT fluorescein is installed to the patient’s eye. The patient is asked NOT to blink, and the tear film is observed under video with a broad beam of blue light. The TBUT is recorded at the time elapsed from the last blink until the appearance of a dry spot is observed in the tear film. A TBUT of under 10 seconds is considered abnormal.
Meibography
Meibography is a scan taken at the eye exam by the optometrist exclusively to look at the health of the meibomian glands. The meibomian glands are the oil secreting tear glands.
Below is an image of healthy meibomian glands, followed by an image of a 35 year old female who developed gland atrophy due to contact lens overwear.
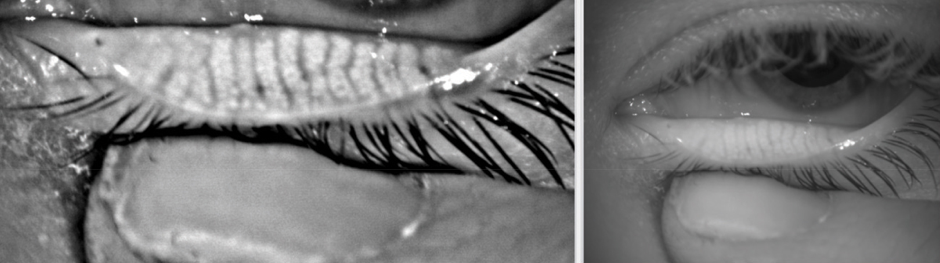
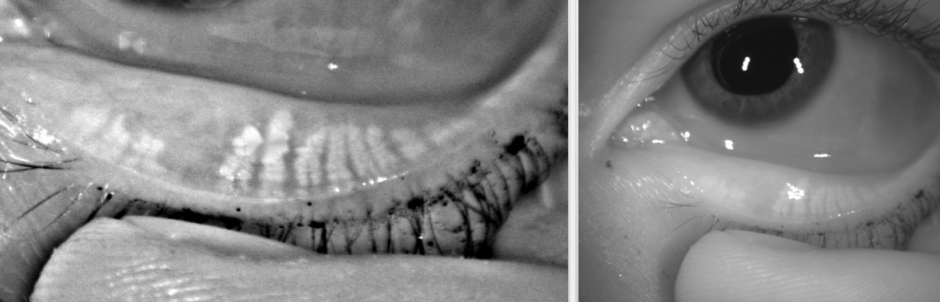
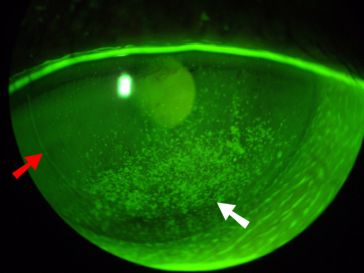
Corneal Staining
The red arrow shows a LASIK scar from laser corrective surgery. The white arrow shows dry patches from fluorescein staining indicating cornea damage.
Different coloured staining agents are applied to the eye by the optometrist to assess:
- Corneal Damage
- Conjunctival damage
- Tear Film instability
Fluorescein sodium dye is more commonly used for corneal staining. Lissamine green dye is more sensitive to conjunctival staining. The staining dyes give an indication of the severity of dry eye and are used to assess improvement of the surface of the cornea following treatment.
Treatment
Tear Supplements & Medicated Eye Drops
There are so many choices at your local pharmacy for dry, red and itchy eyes. But which prescription eye drops do you choose?
Once the optometrist has worked out the cause of the dryness and redness affecting the tear film, the appropriate drops can be recommended. The different causes of dry eye may be due to:
- Lack of oil in the tear
- Lack of tear
- Inflammation of the eye
- Bacterial infection
- Auto-immune systemic conditions
- Drug reaction
- Allergies
Once we know why, it’s a lot simpler to treat the presenting symptoms with the right eye drops. The optometrist can accurately recommend the right treatment plan at the dry eye consultation.
Tear supplements or artificial tears are used to increase the quality and quantity of the tear film. Prevention is the best policy when using tear supplements – often the reason they don’t work is because they are not used frequently enough.
The best times to use tear supplements are as follows:
- Just before going to bed at night
- Upon waking in the morning
- Before concentrated tasks
- Prior to going into the wind or air conditioning
- As soon as the eyes are irritable
Lid Hygiene & Scrubs
This alternative is used to gently remove cosmetics, accumulated oils and crusted material. Cleaning the eyelids reduces the chance of infection, improves contact lens wear and comfort and reduces dry eye symptoms. Cleaning the eyelids removes the build-up of the biofilm layer and bacteria that form at the lid margin. Eyelid cleaning agents include wipes (Systane or Blephadex wipes), foams (Blephadex foam) or diluted baby shampoo.
Warm Compress & Eyelid Hygiene Tips
A warm compress serves to unclog and stimulate the meibomian tear glands. This helps in tear film production and quality.
Warm compresses are recommended 1 to 2 times per day, for approximately 5 minutes each time. Your optometrist will recommend for how long to undertake the warm compresses. The process should be undertaken as follows:
- Place a clean face washer in warm water after washing your hands – as warm as possible without discomfort. It is best not to boil or put the cloth in a microwave to avoid burning the skin.
- Squeeze the excess water. Hold firmly against the closed eyelid for up to 5 minutes.
- As the cloth cools. reheat it in warm water.
- After 5 minutes, massage the eyelid with the cloth. Start from the side closest to the nose and move out to the side closest to the ear.
- Do not use the same face wash on both eyes as this may transfer an infection.
Contact Lenses & Eye Makeup
If you have blepharitis, you should cease wearing contact lens until the blepharitis has resolved. Wearing contact lenses with blepharitis increases your chances of eye infection and more serious eye problems. Once the blepharitis has resolved, consider wearing daily contact lenses to improve the comfort.
As with contact lenses, you should try to minimise your eye makeup wear, such as eyeliner and mascara, until the blepharitis has resolved. The optometrist will let you know and give you the green light to commence using the eye makeup again.
Vitamin Supplements
To keep blepharitis under control, Omega 3 Fatty Acids are recommended to reduced ocular inflammation and improve tear secretion.
